Vaccines, Biotech, and the Modern Moment
Modern vaccination campaigns are, without question, one of the great achievements of medical science. Their origins are, in turn, a case study of the necessity of innovation.
The plagues of the early modern world were many and varied. Smallpox, yellow fever, diphtheria, cholera, pertussis, measles, typhoid, and Yersinia pestis itself tended to spread through entire cities and settlements at lightning speed. Other than quarantine and isolation, the tools available to handle outbreaks were less effective than their practitioners might have wished: prayer, incense, bloodletting, and drinking beer mixed with vinegar were all common.
Although colonizing Europeans spread these diseases around the world, they also began to carry news of techniques for variolation or deliberate preventative infection. While these methods were used in East Asia starting in the 15th century and began to catch on in Europe during the early 18th, the modern concept of vaccination arguably only begins with Edward Jenner’s 1796 experimental proof that the far-milder cowpox could be used in place of actual smallpox. This was brave, dangerous, questionably ethical (his first patient was an eight-year-old child), and utterly, unquestionably brilliant. Nevertheless, his work made inoculation safe and effective for the first time in history.
Two Great Triumphs: Smallpox and Polio
From there, smallpox vaccines swept through colonizing countries even faster than the disease they targeted. By 1801, 100,000 people were vaccinated in Britain alone. The vaccine came to the United States in 1800, to the Spanish Colonies in 1803. By the end of the 19th century, it became mandatory in many countries, with variolation becoming illegal in parallel. Vaccine production became increasingly standardized as essentially an agricultural practice, as cows were needed to produce cowpox serum and, later, the lymph used to deliver it. Air-dried vaccines were developed, then freeze-dried versions in the 1920s. By the 1940s, resources and expertise had expanded to the point that the last few significant outbreaks in America were met with overwhelming public responses: top officials asking residents to attend vaccination clinics, large-scale public funding, lines around the block.
The last natural case of smallpox was recorded in 1977, with a tiny laboratory outbreak in 1978. Since then, the disease’s global eradication has saved an estimated 150-200 million lives. The WHO describes it as the most significant public health achievement in history.
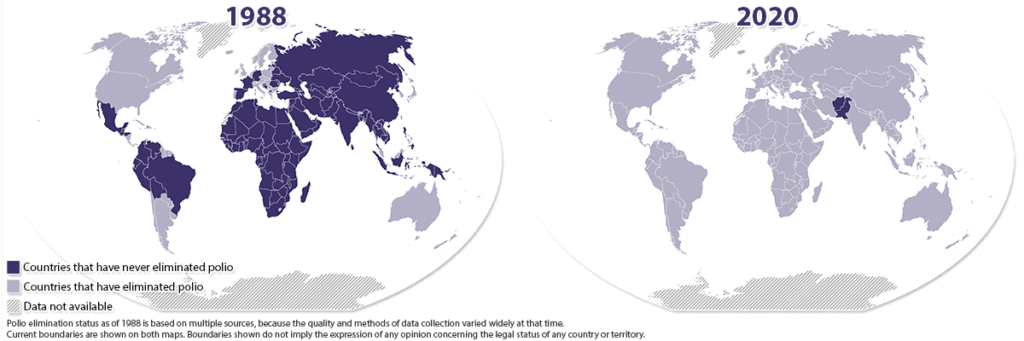
It may soon be matched, however, by the eradication of poliomyelitis. Three wild strains of the poliovirus claimed millions of lives over the 19th and 20th centuries, paralyzing millions more. Two of those strains are now entirely eliminated—one in 2013, the other in 2015—with the third causing a few dozen cases annually in just two countries: Pakistan and Afghanistan. That number is down from an estimated 350,000 annual cases in the late 1980s, of which several thousand cases led to irreversible paralysis and several hundred to death.
That incredible success is due largely to two factors. One is the WHO’s Global Polio Eradication Initiative, which began in 1988 with the ambitious goal of eliminating the disease from 125 countries where it was then endemic. The other is the development of two innovative vaccines: Jonas Salk’s in the early 1950s, which made use of dead poliovirus, and Albert Sabin’s oral vaccine using attenuated poliovirus, approved in 1960. Both were developed with immense public support, championed by an American President who himself had suffered polio as a child, and coming hard on the heels of disastrous earlier vaccine attempts, many of which had infected and paralyzed hundreds of recipients. Because the polio vaccines went into mass production so quickly, they also forced global governments to refine and improve vaccine testing and production processes, providing the foundation for QA techniques that are still in use today.
Between 1800 and the middle of the 20th century, vaccines were developed for the other plagues that defined so much of medieval, early modern, and modern life. Measles, mumps, typhoid, yellow fever, rubella, influenza, diphtheria, pertussis, tuberculosis, cholera, and dozens of other illnesses have been defeated by increasingly sophisticated vaccines using dead, attenuated, or partial viral and bacterial samples. More advanced still are the modern vaccines using RNA or entirely novel non-pathogenic platforms.
COVID-19 and the Fastest Vaccine in History
Over the last 25 months, SARS-CoV-2 has infected more than 400 million people, killing close to 6 million of them. The global medical community has fought back with social and behavioral measures, respirators, antiviral drugs, and 10 billion doses of 20 different vaccines administered to almost 5 billion people. That’s about 62% of the global population, although that number drops to 10.6% in developing nations. As of early 2021, the global vaccine organization GAVI was tracking 63 vaccines in the clinical trial stage, varying from whole virus vaccines to alternatives using protein subunits, viral vectors, and nucleic acid (RNA and DNA).
While major research institutes are still collecting and collating data at a furious rate—and the efficacy of any given vaccine varies tremendously by patient characteristics and disease exposure—it is fair to describe these past two years as the fastest, largest, and most collaborative vaccination project in human history. While estimates vary, unvaccinated people are approximately five times as likely to contract COVID-19 as vaccinated counterparts and seven times as likely to be hospitalised or die. Unfortunately, there are no authoritative estimates of how many lives the vaccines have saved, but the number is undoubtedly in the tens of millions.
The COVID-19 vaccines echo history in one other way, as well. Anti-vaccination leagues first appeared in England in the early 1800s, just a few years after Edward Jenner’s vaccine began to be widely administered. Then as now, some objections were reasonable—that early vaccine was a far more invasive medical procedure than a modern injection—while others were spurious, such as the belief that diseases were spread by miasma, causing concern that the vaccine would be ineffective. The most enduring complaint, however, is one we still see today. Some citizens argued that compulsory vaccination, even one necessary to combat the deadliest disease of their time, was a violation of personal liberty. These disputes became legal battles and eventually led to the US Supreme Court’s first ruling on the power of states to compel vaccination. That was in 1905.
If we can just succeed in overcoming our modern version of those same challenges, the COVID-19 vaccines will enter history as a victory on par with our triumphs over smallpox, polio, and their cousins.
Jennifer Phillips originally wrote this article. Have questions? Get in touch!
—
Note: Unless otherwise specified, the information above comes either from the US CDC or from the College of Physicians of Philadelphia.
Ready to realize your future?